The Centers for Medicare & Medicaid Services (CMS) use patient feedback about their care as part of their reimbursement plan for acute care hospitals. Under the Hospital Value-Based Purchasing Program, CMS makes value-based incentive payments to acute care hospitals, based either on how well the hospitals perform on certain quality measures or how much the hospitals’ performance improves on certain quality measures from their performance during a baseline period. This program began in FY 2013 for discharges occurring on or after October 1, 2012.
A standard patient satisfaction survey, known as HCAHPS (Hospital Consumer Assessment of Healthcare Providers and Systems), is the source of the patient feedback for the reimbursement program. I have previously used these publicly available HCAHPS data to understand the state of affairs for US hospitals in 2011 (see Big Data Provides Big Insights for U.S. Hospitals). Now that the Value-Based Purchasing program has been in effect since October 2012, I wanted to revisit the HCAHPS patient survey data to determine if US hospitals have improved. First, let’s review the HCAHPS survey.
The HCAHPS Survey
The survey asks a random sample of recently discharged patients about important aspects of their hospital experience. The data set includes patient survey results for US hospitals on ten measures of patients’ perspectives of care. The 10 measures are:
- Nurses communicate well
- Doctors communicate well
- Received help as soon as they wanted (Responsive)
- Pain well controlled
- Staff explain medicines before giving to patients
- Room and bathroom are clean
- Area around room is quiet at night
- Given information about what to do during recovery at home
- Overall hospital rating
- Recommend hospital to friends and family (Recommend)
For questions 1 through 7, respondents were asked to provide frequency ratings about the occurrence of each attribute (Never, Sometimes, Usually, Always). For question 8, respondents were provided a Y/N option. For question 9, respondents were asked to provide an overall rating of the hospital on a scale from 0 (Worst hospital possible) to 10 (Best hospital possible). For question 10, respondents were asked to provide their likelihood of recommending the hospital (Definitely no, Probably no, Probably yes, Definitely yes).
The Metrics
The HCAHPS data sets report metrics for each hospital as percentages of responses. Because the data sets have already been somewhat aggregated (e.g., percentages reported for group of response options), I was unable to calculate average scores for each hospital. Instead, I used top box scores as the metric of patient experience. I found that top box scores are highly correlated with average scores across groups of companies, suggesting that these two metrics tell us the same thing about the companies (in our case, hospitals).
Top box scores for the respective rating scales are defined as: 1) Percent of patients who reported “Always”; 2) Percent of patients who reported “Yes”; 3) Percent of patients who gave a rating of 9 or 10; 4) Percent of patients who said “Definitely yes.”
Top box scores provide an easy-to-understand way of communicating the survey results for different types of scales. Even though there are four different rating scales for the survey questions, using a top box reporting method puts all metrics on the same numeric scale. Across all 10 metrics, hospital scores can range from 0 (bad) to 100 (good).
I examined PX ratings of acute care hospitals across two time periods. The two time periods were 2011 (Q3 2010 through Q2 2011) and 2013 (Q4 2012 through Q3 2013). The data from the 2013 time-frame are the latest publicly available patient survey data as of this writing.
Results: Patient Satisfaction with US Hospitals Increasing
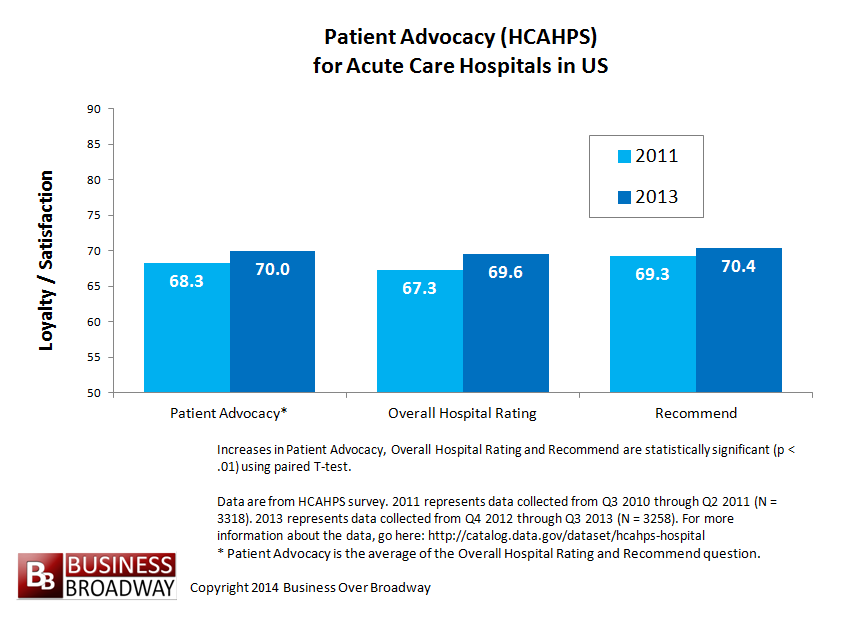
Figure 1 contains the comparisons for patient advocacy ratings for US hospitals across the two time periods. Paired T-tests comparing the three loyalty metrics across the two time periods were statistically significant, showing that patients are reporting higher levels of loyalty toward hospitals in 2013 compared to 2011. This increase in patient loyalty, while small, is still real.
Greater gains in patient loyalty have been seen for Overall Hospital Rating (increase of 2.26) compared to Recommend (increase of 1.09).
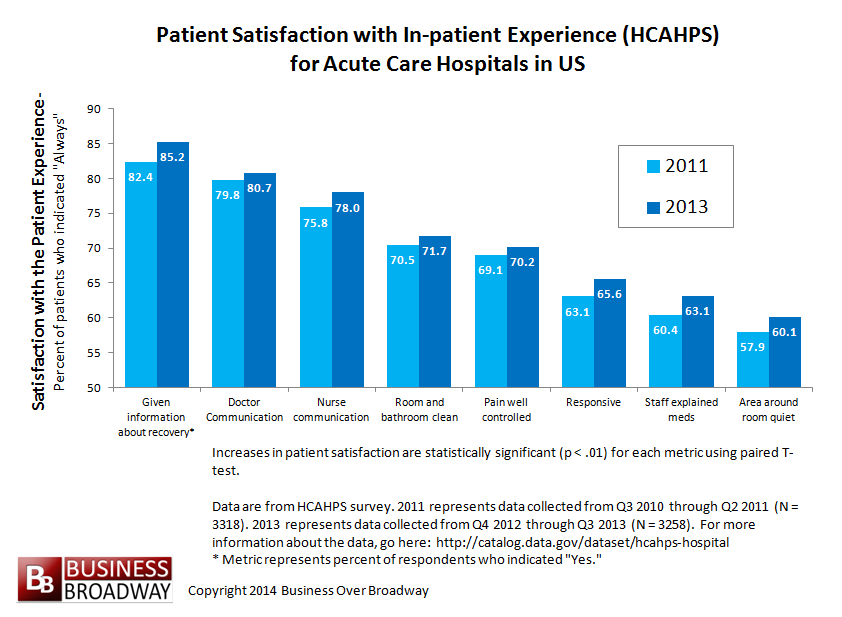
Figure 2 contains the comparisons for patient experience ratings for US hospitals across the two time periods. Again, paired T-tests comparing the seven PX metrics across the two time periods were statistically significant, showing that patients are reporting higher levels of satisfaction with their in-patient experience in 2013 compared to 2011.
The biggest increases in satisfaction were seen in “Given information about recovery,” “Staff explained meds” and “Responsive.” The smallest increases in satisfaction were seen for “Doctor communication” and “Pain well controlled.”
Summary
Hospital reimbursements are based, in part, on their patient satisfaction ratings. Consequently, hospital executives are focusing their efforts at improving the patient experience.
Comparing HCAHPS patient survey results from 2011 to 2013, it appears that hospitals have improved how they deliver patient care. Patient loyalty and PX metrics show significant improvements from 2011 to 2013.